Drug-Resistant Malaria Appears in the U.K.
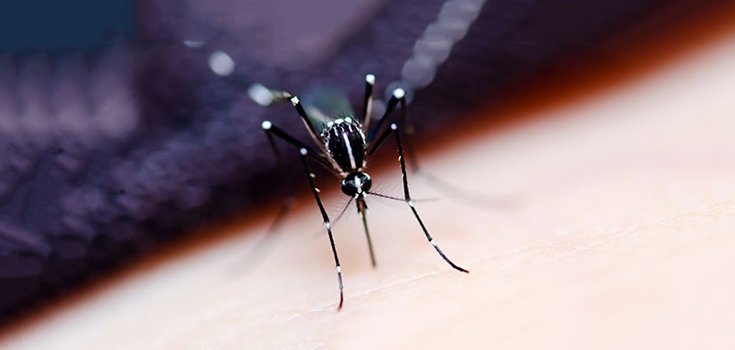
Malaria used to be easily treatable in the United Kingdom, but things have become more complicated since a drug-resistant strain of the disease popped up.
Doctors give patients with “uncomplicated” malaria an artemisinin-based drug combination called Artemether-lumefantrine. After 3 or 4 days of taking the pills, the malaria parasites are killed off and the patient feels better.
Over the past 15 years or so, artemisinin has become the gold standard of treatment for the most common malaria infections both in British hospitals and throughout much of the developing world. [1]
But the malaria parasites have been adapting to the drugs, rendering them useless. Artemisinin-resistance has been slowly developing in Southeast Asia, and it appears they’re starting to lose their punch in Africa, as well.
Health officials in Britain first stumbled across a cluster of malaria cases resistant to Artemether-lumefantrine in patients who had returned from 3 different African countries – Angola, Liberia, and Uganda. The drug appeared to cure the travelers. [2]
But the success was short-lived, and the parasites returned about a month later.
The 4 individuals had to seek alternative treatment, the London School of Hygiene and Tropical Medicine said in new study.
Colin Sutherland, a medical researcher from the LSHTM, said:
“It may be an early warning that we need to change a few things.” [3]
Sutherland had heard colleagues from Africa discussing their own experiences with parasites resistant to the drug. Based on their observations, the cases seem to be developing in different parts of the continent slowly.

The researchers say there’s no need to panic just yet, but to expect that things could get worse. They are demanding more research into the efficacy of the Artemether-lumefantrine drug. [2]
Said Sutherland:
“It’s remarkable there’s been four apparent failures of treatment, there’s not been any other published account [in the UK].
It does feel like something is changing, but we’re not yet in a crisis. It is an early sign and we need to take it quite seriously as it may be snowballing into something with greater impact.”
Samples of the parasites indicated that they had evolved different mechanisms for survival, rather than there being 1 new type of resistant malaria parasite spreading through Africa.
Read: GM Mosquitoes Being Created to End Malaria…or Spread it?
Professor Dame Sally Davies, the chief medical officer for England, said:
“This is a stark warning for the future of global medicine.
We are in dire need of new drugs to keep pace with resistance, in low and middle-income countries in particular, the consequences of ineffective drugs are catastrophic.”
Malaria is a mosquito-borne disease that is a major killer of children under 5, with 1 child dying from the disease every 2 minutes. Sub-Saharan Africa is home to 90% of the world’s malaria cases, and 92% of malaria deaths. [3]

World Health Organization (WHO) data shows there were more than 200 million cases in 2015, and roughly 430,000 deaths. [1]
Sources:
[1] NPR
[2] BBC News
[3] Reuters
