“Smart” Bandages Could Slow the Spread of Superbugs
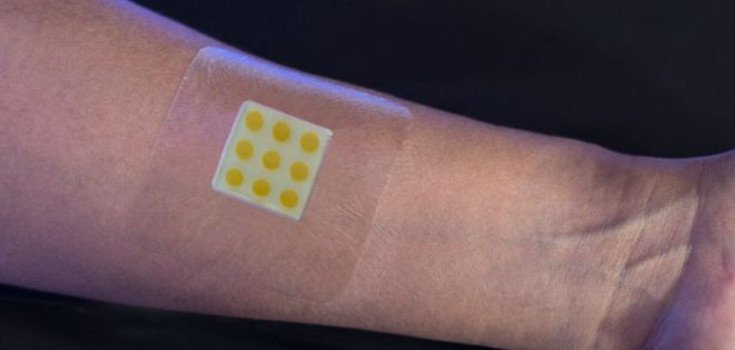
A new “smart” bandage developed by Australian scientists may help stop the spread of drug-resistant bacteria by alerting doctors when a wound develops an infection.
The bandage alerts a patient or healthcare provider to problems with a wound by changing color, and can automatically release an antibiotics contained within polymer capsules. The color itself is released by fluorescent housed in capsules when toxins are detected. The device is connected via Bluetooth to a smartphone, and sensors in the bandage can alert a doctor if toxic bacteria are present. [1]
The new technology would prevent doctors from doling out antibiotics when they are not truly needed.
Scientists say the dressings could be especially useful in the treatment of children with burns, as they are more susceptible to bacterial infections due to their immature immune systems. Burn-related infections can slow the healing of wounds, resulting in longer hospital stays and often permanent scarring. Such infections can also be deadly.
It can be difficult for doctors to diagnose an infection without removing a patient’s dressing, which is often a painful process that results in even more scarring. Antibiotics are often prescribed to burn patients and patients with other severe wounds as a preventative measure, but antibiotics are over-prescribed and researchers fear that drug-resistant “superbugs” could one day render antibiotics useless, killing tens of thousands of people. Frighteningly, that day might not be too far off.
The bandages could slash the $3 billion annual cost of wound treatment in Australia. [2]
The Medical Research Council has awarded the Australian scientists a hefty grant to test the responsiveness of the prototype dressing to samples taken from burn victims’ wounds.
The scientists presented the dressing at a Melbourne forum in August.
Researchers from University of Tokyo’s Graduate School of Engineering are working on a similar device that is supposedly able to function with minimal electrical power, which they say actually boosts the signal of the bandages’ readings. The dressings can be printed out and made of “molecules that bond together to form a polymer chain.” [3]
In April, Livescience reported that a team of researchers from Harvard, Purdue, Tufts and Brigham and Women’s Hospital were bringing together advances in sensors, biomaterials, tissue engineering, microsystems technology and microelectronics to create their own smart bandages.
The flexible biometrics, as the team refers to it, would go beyond simply notifying doctors and patients of infections and delivering antibiotics. The devices would also be able to monitor all the vital signs of the healing process, such as oxygen levels and temperature, and make adjustments when needed, as well as communicate the information to health professionals who are off-site.
Reza Abdi, associate professor of medicine at Harvard and a part of the research team, told the publication:
“The goal is to have a smart band-aid system using flexible sensors and electronics. Current wound care or band-aid technology is designed to protect the wound area from environmental assault. However, it is a simple technology, which does not provide any information about the state of the wound.
Our goal is to embed sensors and electronics to band-aids which will enable real-time monitoring of the wound environment and in case of a need, and intervene to remedy the external conditions (infection, etc.) by delivering drugs. We anticipate that such band-aids may be used on patients within five to ten years.” [4]
Sources:
[1] BBC News
[2] Herald Sun
[3] HNGN
[4] Livescience

would this be a successful way to detect Lyme disease? Since the current test are crap, we really need something that works so people don’t go undiagnosed for so long. it would end so much suffering and would end doctors labeling and prescribing meds for symptomatic diagnoses.