First Cases of Drug-Resistant Candida Auris Spreading in US Hospitals
Thirteen people in the United States have been infected with a potentially deadly, drug-resistant fungal infection since 2009, health officials say. [1] [2]
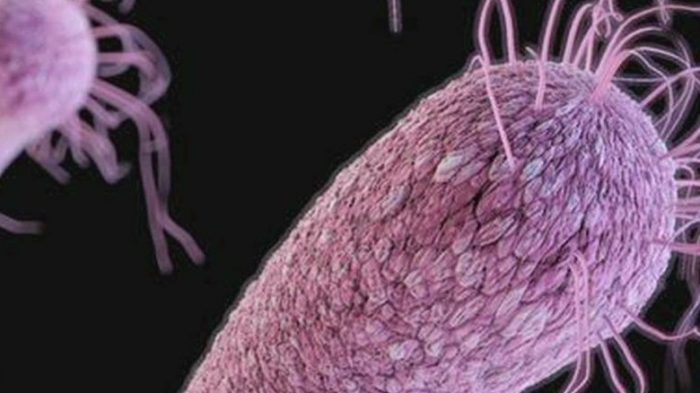
Of those infected, 4 individuals died; but it is not clear whether they died from the infection or from other underlying health problems. [1]
Dr. Tom Chiller, who is chief of the mycotic diseases branch of the U.S. Centers for Disease Control (CDC), said:
“I am worried. I think this is a real threat.” [2]
The infection, Candida auris, is a growing global health threat and appears to spread within hospitals and other healthcare facilities, CDC officials said. [1]
In an agency statement, CDC Director Dr. Tom Frieden said:
“We need to act now to better understand, contain and stop the spread of this drug-resistant fungus. This is an emerging threat, and we need to protect vulnerable patients and others.”
The 13 cases were reported in Illinois, Maryland, New Jersey, and New York. All the individuals were hospitalized for underlying health problems an average of 18 days before being diagnosed with C. auris. Two individuals who had been treated in the same hospital or care facility were diagnosed with nearly identical fungal strains. This fact is what leads health officials to believe that patients are acquiring the infection in hospitals and healthcare facilities.
The CDC sounded the alarm about the worldwide spread of C. auris back in June and asked laboratories to report cases and send patient samples to state and local health departments, as well as to the CDC.
In the months since issuing the alert, the CDC has been investigating reports of the fungal infection with several state and local health departments. Health officials expect more cases to emerge as knowledge of C. auris grows and investigators dig through patient samples.
C. auris can be easily misdiagnosed as a regular Candida infection. Specialized laboratory testing is required to differentiate the two types of yeast. This often means that patients don’t receive appropriate treatment.
Causing further alarm, the CDC said that 71% of C. auris strains from U.S. patients have some resistance to anti-fungal drugs.
Additionally, some of the strains identified in the U.S. patients were related to strains in South Asia and South America, but none of the patients had traveled to or had direct links to those areas, suggesting that they acquired the infections locally.
The Mechanics of C. auris
C. auris causes dire wound and bloodstream infections in hospitalized patients. It acts like other serious healthcare-associated infections like MRSA, Klebsiella, and Acinetobacter. These bugs are transferred to patients via healthcare workers’ hands and contaminated hospital equipment. [2]
And, like these bacteria, the fungus overwhelms the immune system and resists drug treatment. This was formerly unheard of in fungi, particularly yeasts.
In the type of Candida infection normally associated with hospitals and nursing homes, candidemia, yeasts live within the intestines, where they cause few to no problems. The yeasts become harmful yeast infections when they leak into the bloodstream and cause a whole-body infection that can become life-threatening. In these cases, people are the sources of their own infection.
C. auris works more like MRSA and other potentially deadly bacteria, in that it is spread to patients via the hospital environment, including catheters, countertops, and other surfaces. Candidemia infections can’t be spread from person to person, but C. auris can cause outbreaks.
There are only three classes of anti-fungal drugs (compared to more than a dozen families of antibiotics); and not only are these medications in short supply, but C. auris is showing resistance to all of them.
Who is at Risk?
People who have serious underlying health problems and/or are being treated in a hospital or other healthcare facility are most at-risk for acquiring a C. auris infection. These individuals are typically taking numerous drugs, which have weakened their immune systems. Such patients are touched by many doctors, nurses, and other healthcare workers, who could easily transfer the fungus to the skin.
Chiller said:
“We consider this a serious threat that we want to act on aggressively. It is just not acting like a typical Candida. The fact that it is being transferred so readily in hospitals, the fact that it can develop really bad resistance, and the fact that it is hard to identify make it a real threat and a challenge.”
Sources:
[1] HealthDay
