It’s Here: Bacteria Resistant to ALL Antibiotics Shows Up In U.S.
For the past several months, I’ve been writing about a superbug that is resistant to all antibiotics, including “last resort” drugs. Experts first found it in China, and believed it would take about a decade to cross over into Europe. However, they were wrong; it only took a few months. It also arrived in Canada, and now it’s here, too.
The woman went to a clinic in Pennsylvania in April seeking care for a urinary tract infection, and the clinic forwarded a sample to Walter Reed National Military Medical Center in Bethesda, Maryland. Walter Reed discovered the superbug in her urine. It is not known how the bacteria got into the woman’s system; she has not traveled outside of the U.S. in the past 5 months. This would suggest that more people in the United States are infected with the bacteria.
The CDC and the Pennsylvania State Health Department are investigating the case and working to trace the contacts the woman have had to see if the bacteria had spread. The CDC also said it was looking for other potential cases of the superbug in the health care facility that treated the patient. [1]
The strain of E. coli which infected the woman is resistant to all antibiotics, including colistin, the “big gun” that doctors pull out of their arsenal when all other drugs fail. Colistin was approved in the 1950s but fell out of favor in the 1970s because of its toxicity, USA Today reports. It is only used when absolutely necessary.
The superbug is now present in more than 2 dozen countries. Given the danger of colistin-resistant bacteria, doctors at Walter Reed decided to start testing samples from the U.S. Patrick McGann, a senior microbiologist at the Walter Reed National Military Medical Center, said:
“People have begun looking for it. And now that they’re looking for it, they’re finding it. It’s only a matter of time before these bacteria start showing up.”
Read: 2 Main Contributors to the Antibiotic-Resistant Crisis
Fortunately, the Pennsylvania woman’s infection was susceptible to a handful of antibiotics, including a class called carbapenems, so her infection was treatable.
Frieden said:
“We risk being in a post-antibiotic world. The medicine cabinet is empty for some patients.”
Bacteria become resistant to antibiotics in 2 ways. Some acquire mutations in their own genomes that allow them to resist the drugs. This ability can’t be shared with pathogens outside their own family.
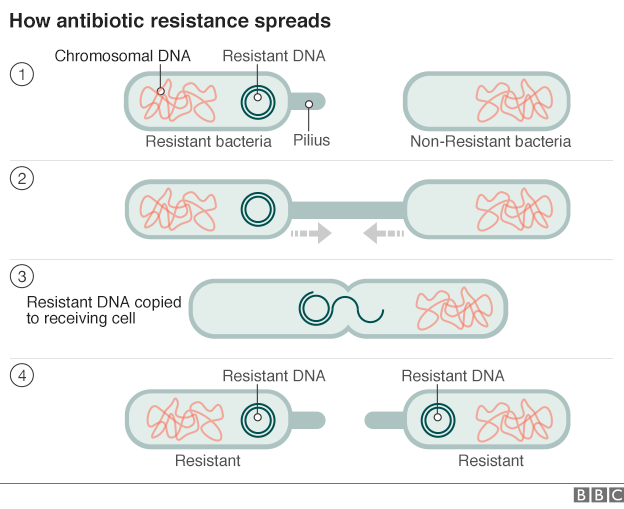
The bacteria inside the Pennsylvania woman, however, became “infected” with a plasmid – a small piece of DNA carrying a gene for antibiotic resistance. These bacteria are more dangerous because plasmids can duplicate themselves and transfer the genes they carry to other bugs within the same family, as well as to other families of bacteria, which can then “catch” resistance directly without having to develop it through evolution, The Washington Post explains.
David Hyun, a senior officer leading an antibiotic-resistance project at the Pew Charitable Trust, said:
“This is definitely alarming. The fact that we found it in the United States confirms our suspicions and adds urgency to actions we need to work on antibiotic stewardship and surveillance for this type of resistance.”
Read: 5 Natural Antibiotic Solutions for Antibiotic-Resistant Infections
By 2050, antimicrobial resistance could kill 10 million people a year – more than cancer. Time is running out to save modern medicine. Last week, economist Jim O’Neill published an 84-page document laying out 9 interventions, but it’s already being met with resistance.
Last year, Congress agreed to allocate hundreds of millions of dollars to the federal agencies at the frontlines of the battle against antimicrobial resistance. More than $150 million is set to go to the CDC to assist state and local health departments to prevent and monitor superbug outbreaks.
But others must join the battle, including doctors and meat producers. In the United States, in 1 in 3 prescriptions for antibiotics are unnecessary. And while some meat companies are actively working to reduce or cut the number of antibiotics they feed their animals, far too many continue to give the drugs to livestock to prevent illness and promote growth.
That’s how this particular bacteria became resistant to colistin – international farmers regularly fed them to animals. Humans then eat those animals, consume their milk, and the animals’ waste seeps into groundwater.
Sources:
[1] CNN
