Study: People Save Antibiotics for Later Use, and it is Not Good
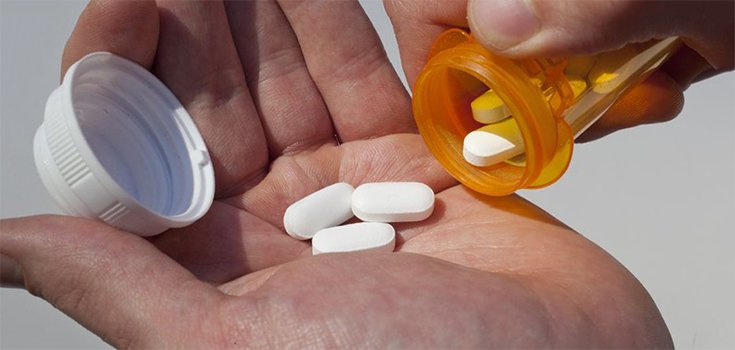
Many people in the United States hang on to leftover antibiotics and say that if they got sick, they’d use them without going to the doctor, a new study finds.
The findings are so problematic, it’s hard to even know where to begin. However, one of the main concerns is that this practice leads people to take the drugs when they might not need them, which may further the spread of resistance to antibiotics.
Dr. Larissa Grigoryan, an instructor of family and community medicine at Baylor College of Medicine in Texas, said in a statement:
“When people self-diagnose and self-prescribe antibiotics, it is likely that the therapy is unnecessary, because most often, these are upper-respiratory infections that are mostly caused by viruses.”
Antibiotics do not kill viruses.
Moreover, if someone has “leftover” antibiotics, it means they didn’t take the full course prescribed to them, which may also further the spread of antibiotic resistance.
And not all antibiotics were created equal. If you choose to take leftover drugs, and you actually do have a bacterial infection, you might not be taking the right type of antibiotic to treat it.
For the study, Grigoryan and her colleagues analyzed information from 400 patients who went to family practice clinics in Houston and were surveyed about their use of antibiotics.
As reported by LiveScience,
“Among those who said they stored antibiotics at home, 74% said these drugs were leftover from a previous prescription.” [1]
Grigoryan said:
“The most common conditions patients reported self-treating with antibiotics were sore throat, runny nose, or cough–conditions that typically would get better without any antibiotic treatment.”
Among patients who said they would use an antibiotic without a prescription, 60% went to public clinics that provide care for underserved minority patients, 44% of whom reported annual incomes of less than $20,000.
Grigoryan explained:
“Patients from public primary care clinics, those with less education, and younger patients had a higher risk of [non-prescription] use in our survey.”
Many of these individuals are self-prescribing to save money on drugs and co-pays, the authors theorize, as the co-pays in public clinics ranged up to more than $70. [2]
Fueling Antibiotic Resistance
Increasingly, efforts are being made to reduce the number of unnecessary antibiotic prescriptions from doctors. However, the findings of the study suggest that greater attention should be paid to making sure antibiotics are taken properly, and to the problem of people taking the drugs without a prescription.
Antimicrobial resistance spreads among different bacterial species. According to the CDC, at least 2 million Americans are infected with drug-resistant pathogens every year, and 23,000 die from the infections. [2]
Plasmids – small pieces of DNA carrying genes for antibiotic resistance – can duplicate themselves in pathogens and transfer the genes they carry to other bugs within the same family, as well as to other families of bacteria.
In May, the CDC revealed that a bacterium resistant to all antibiotics had been found in the U.S.
A second case of the superbug was found in the U.S. in June.
Experts have warned that if we don’t get a handle on the problem, antimicrobial resistance could eventually kill more people than cancer.
Sources:
[1] LiveScience
[2] ScienceDaily
