Brain Scans may Predict Depression Relapse
A simple functional magnetic resonance imaging (fMRI) scan could help doctors predict which patients might be at risk of relapsing into depression.
Researchers from King’s College London and the University of Manchester conducted a small study of 64 patients who were in remission from major depressive disorder, none of whom were prescribed medication. The scientists conducted an fMRI on the patients to search from atypical connections in the brain.
The participants were asked during the fMRIs to envision treating their best friends poorly, which caused them to experience guilt and other self-blaming emotions. Researchers followed up with the patients over the next 14 months and monitored them for symptoms of depression. Thirty-seven of the participants were depression-free at the end of the study, and 27 had relapsed.
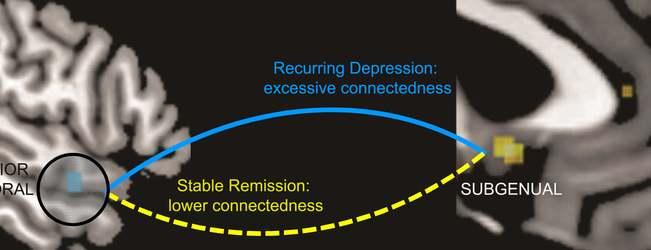
The fMRIs of the relapsed participants showed increased connectedness between the anterior temporal lobe and the subgenual region – the sections of the brain that are linked with feelings of guilt. Researchers saw no increase in connectedness in the brains of those who remained depression-free at the conclusion of the study. [1]
Next, the team tested the approach on a control group of 39 people with no family history of major depression and found that they, too, showed no increased connectedness.
Based on the level of connectedness observed in the fMRIs, the scientists were able to predict which participants would relapse with an overall accuracy of 75%. [2]
Read: 7 Natural Solutions for Alleviating Depression
“This is the first study to show that fMRI can be used to make predictions about who will develop depression in the future, once they’ve recovered from a previous episode. These findings could mean that fMRI could help doctors make better decisions about who should continue their antidepressants and who should stop them,” said Dr. Roland Zahn, lead researcher based at the Institute of Psychiatry, Psychology & Neuroscience (IoPPN), King’s College London.
“Before this approach can be rolled out and used in the clinic, we need to test it out in an independent group of patients and improve it, so that its accuracy reaches 80 per cent. If future studies can reach this mark, then this approach will be vitally important as there are currently no accurate ways to predict those who will have a recurrence following recovery,” Dr. Zahn said.
All of this means that the potential is there to identify at-risk patients and to treat them with long-term antidepressants to prevent them from sinking back into the misery of depression, an illness that affects some 15.7 million adults in the U.S. aged 18 and older.
The study is published in the journal JAMA Psychiatry.
The question is, will treating these patients with long-term antidepressants help or hurt them?
In July, we reported that antidepressants may cause permanent brain damage, as they treat the symptoms of depression, but not the underlying cause.
Additionally, a 2011 study found that people who take antidepressants have a greater risk of relapse than people who don’t. Specifically, those who had never taken the medications were found to have a 25% chance or relapse compared to 42% or higher in those who had used the drugs. [3]
Sources:
[1] GlobalPost
[3] PsychCentral
