Automated Insulin System Approved for People with Type 1 Diabetes

Life is about to get easier for people with Type 1 diabetes, now that the U.S. Food and Drug Administration (FDA) has approved a new automated insulin delivery system.
In Type 1 diabetes, the pancreas makes little or no insulin, so patients must inject themselves multiple times a day with insulin, or use an insulin pump. It can be easy to inject too much or too little of the hormone, depending on what and how much a person eats, and if they exercise. [1]
High levels of blood glucose (sugar) can lead to organ damage, but injecting too much insulin can lead to a dramatic sugar drop that can cause unconsciousness or coma. [1]
The new device prevents both scenarios from occurring.
Type 1 Diabetes: A Few Facts
Type 1 diabetes affects about 1.25 million Americans. It is often caused by genetics, and sometimes exposure to specific viruses. People with the disease have a life expectancy that’s 12.2 years less than the general population. [2]
People with both Type 1 and Type 2 diabetes have an increased risk of:
- Hypertension
- Unhealthy cholesterol levels
- Heart attack
- Stroke
- Blindness and eye problems
- Kidney disease
- Amputations [3]
The New Device
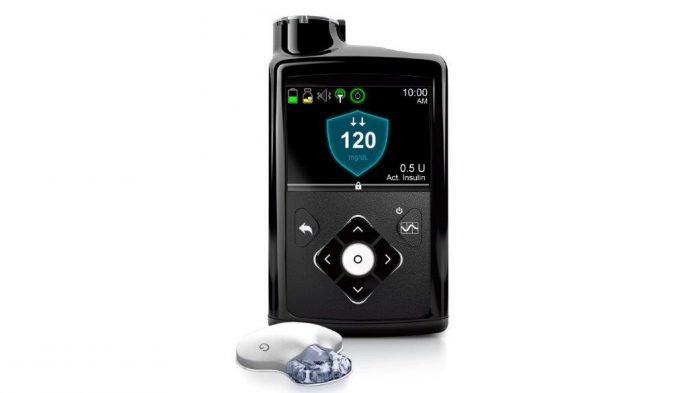
The FDA just approved the MiniMed 670G hybrid closed loop system, made by Medtronic, which consists of an insulin pump and continuous glucose monitor. Both are currently on the market and sold separately. [1]
Read: Artificial Pancreas May be Available for Type 1 Diabetes Patients by 2018
Medtronic’s earlier system also included a feature that would shut down the insulin pump if the wearer’s blood sugar dropped too low. However, the new system actually predicts when an individual’s blood sugar is dropping and prevents it from crashing in the first place. It also corrects high blood sugars.
The 679G has been given the moniker “artificial pancreas” because it essentially does what the real thing would do.
The MiniMed 670G, approved for users age 14 and up, measures a patient’s blood glucose levels every 5 minutes and administers insulin on an as-needed basis.
The system uses a sensor with a protruding needle that slips under the skin and measures insulin levels, while an insulin pump the size of a smartphone that is worn on the abdomen delivers the insulin via tubes that lead to a catheter. [2]
Unlike a real pancreas, however, users must still program the device to deliver extra insulin during meal time, and will have to make adjustments when exercising, which can make insulin levels drop. [2]
The device must be recalibrated every 12 hours, and the glucose sensor swapped out once a week.
If you don’t have diabetes, or don’t intimately know someone that does, all of this might sound like a ton of work and not much of an “advancement.”
But it’s much better than repeatedly stabbing yourself in your fingers to test your blood glucose, and having to inject insulin all the time. As a diabetic, I know of whence I speak.
Furthermore, people with Type 1 diabetes who use the device will be able to sleep through the night without worrying about their sugar levels dropping, and not have to constantly worry about their glucose throughout the day.
The MiniMed 670G was tested on more than 120 patients, and at the conclusion of the study, the average HbA1c blood sugar level of the patients had fallen from a baseline of 7.4% to 6.9%, with nearly 3 in 5 patients (58%) achieving an HbA1c below 7%. HbA1c reflects average blood glucose levels over an 8- to 12-week span.
Said Aaron Kowalski, chief mission officer for the JDRF, the organization that funds much of the “artificial pancreas” research:
“You get almost normalized overnight blood glucose. For people with Type 1 diabetes, that’s massively important. The diabetes isn’t gone, but [wearers] can think about it less …This is a historic milestone.” [1]
Sources:
[1] KQED
[2] The Motley Fool
